Stomatitis during antibiotic therapy – case report
Ulcerative and erosive lesions that appear on the oral mucosa are a common cause of pain, cause difficulties in food intake and pose a problem in maintaining proper oral hygiene.
The etiology of these types of lesions should include local factors, such as trauma to the oral cavity caused by e.g. damaged fillings, untreated tooth decay, braces, denture brackets, para-functions, and even brushing or flossing teeth. General factors include infectious diseases of bacterial, viral, fungal origin, conditions associated with vitamin and micronutrient deficiencies and diseases that cause a decline in immunity. Also, prolonged fatigue and stress, especially chronic stress, can promote the appearance of oral mucosal lesions [11,12].
In the presented paper we will present a clinical case of oral mucositis in a young patient during antibiotic therapy.
Patient A.J., aged 24, came to the office with symptoms of oral mucositis, which appeared during oral antibiotic therapy used for a throat infection. The patient had been taking Duracef in 5ml suspension, 2 times a day, for 4 days. Painful lesions appeared on the oral mucosa during therapy.
In her history, the patient reported malaise and swelling and burning of the tongue, as well as self-induced pain, increasing both during food intake, speaking and during oral hygiene procedures. The patient did not have a fever. She gave no history of comorbidities, and had not previously observed lesions of a similar nature in the oral cavity [10].
Due to difficulties in food intake, the patient noticed weight loss of approx. 2 kg. According to the patient, the biggest problem was pain, significant swelling and burning of the tongue, and severely hampered daily activities such as eating, speaking and maintaining oral hygiene.
An intraoral examination revealed:
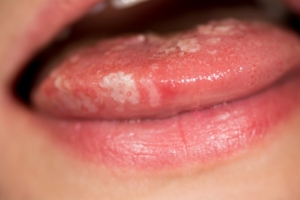
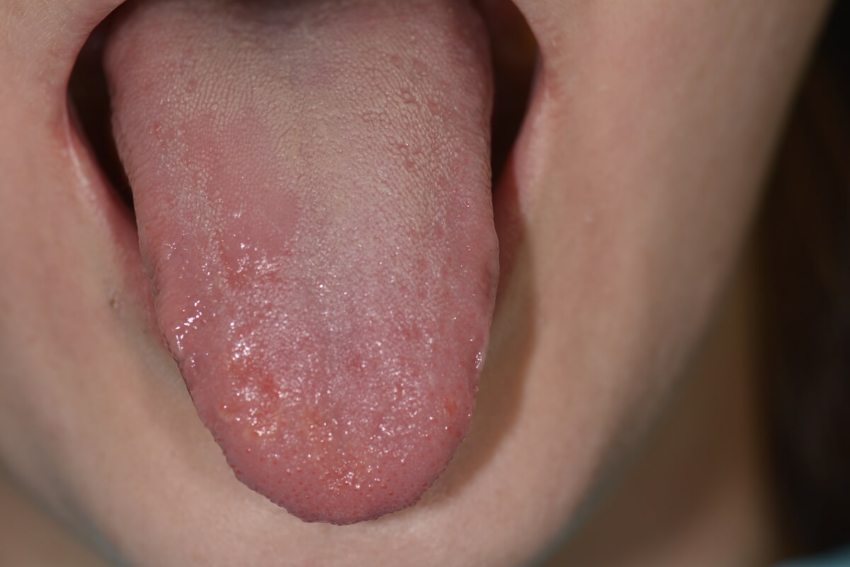
– lesions of aphthous-like eruptions and erosions on the dorsum and edges of the tongue,
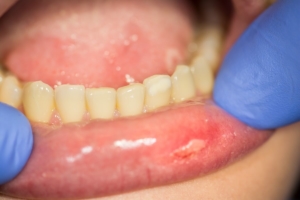
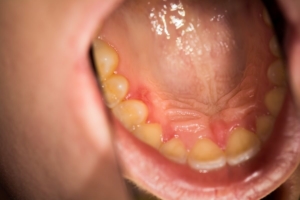
– aphthous and erosive lesions on the oral mucosa (single aphthous lesions located on the mucosa of the lower lip and in the oral vestibule in the area of teeth 44-45, as well as on the mucosa of the alveolar process of the mandible in the area of the lower incisors on the lingual side, erosions on the mucosa of the palate in the area of teeth 14, 15, 27, 28).
The patient’s dentition showed no decayed teeth or abnormal fillings that could be a traumatic cause of the oral lesions. Deterioration of oral hygiene related to the local condition was noted.
Palpation examination assessed the status of the submandibular and submandibular lymph nodes, which were enlarged, painful and displaced relative to the ground.

Disorders of the body’s homeostasis are influenced by systemic diseases, stress, fatigue, inadequate diet, or taking medications, including antibiotics [1,13]. To restore the body’s balance, it is necessary to strive to remove the cause and implement appropriate treatment.
A common complication, both during and after antibiotic therapy, is intestinal dysbiosis, which is associated with an imbalance of the intestinal microbiota. This creates an overgrowth of potentially pathogenic microorganisms, with a concomitant reduction in the normal intestinal flora [9]. Associated with intestinal dysbiosis is oral candidiasis, which is encountered in dental practice, where opportunistic infection with Candida yeasts occurs.
A rare but serious systemic complication is pseudomembranous enteritis associated with oral antibiotic therapy with e.g. The lincosamide group (Dalacin, Clindamycin), which are often ordered in dentistry.
In treating oral mucosal lesions, it is important to eliminate the cause and then implement local and general treatment. An extremely important and often underestimated role in treatment by doctors is played by probiotic therapy during and after antibiotic therapy [7].
The general treatment we used was designed to have an immunomodulatory effect and induce changes in the intestinal microbiotic profile to minimize the side effects of antibiotic therapy.
General treatment which was applied to the patient consisted of taking Enterol once a day for 2 weeks. Enterol contains freeze-dried eukaryotic yeast Saccharomyces boulardii strain CNCM – i745, which is antibiotic-resistant and a natural bioregulator of the intestinal microbiota [14]. The patient then took Vivomix capsules 1x daily for 2 months. The formula in its composition contains lyophilized live cultures of Lactobacillus, Bifidobacterium, and Streptococcus. Prolonged probiotic supplementation after the end of antibiotic therapy provides the opportunity to rebuild the intestinal ecosystem [1,4,5,6,8].
Lactoferrin in 2×1 sachets was also prescribed until symptoms resolve, as well as vitamin A+E, vitamin D3, B vitamins and Omega 3 acids.
The patient was given dietary recommendations and oral hygiene instructions. Laser biostimulation was also ordered for aphthous and erosive lesions, but the patient did not continue laser therapy due to the distance of the office from her residence [11].
Antibiotic therapy was continued for 6 days only, due to the occurrence of local complications in the oral cavity, as well as the onset of diarrhea.
In the initial stage of topical treatment The patient used chlorhexidine in mouthwash and Nystatin in suspension for brushing the oral cavity, ordered by her family doctor.
Liquid chlorhexidine used at this stage of topical treatment caused excessive burning of the tongue mucosa, and Nystatin also showed a similar effect, which became the reason why the patient stopped using both preparations.
According to. Literature Nystatin in suspension is the drug most commonly used for the topical treatment of candidiasis lesions, but it is increasingly unsuccessful [3].
To alleviate pain, a topical analgesic and anti-inflammatory drug product called Glimbax was included, which the patient used 3 times a day for 5 days. The preparation, whose main ingredient is diclofenac, was well tolerated by the patient, and the lack of alcohol in the formulation did not increase burning sensation on the tongue.
According to the drug product characteristics, liquid diclofenac penetrates the oral mucosa very well and accumulates relatively easily in inflamed tissues. At the same time, applied topically, it is minimally absorbed into the bloodstream and has virtually no systemic effect [14].
The use of Glimbax in the topical treatment of oral mucositis has greatly improved the patient’s daily comfort, with reduced swelling of the tongue and less pain at the sites of mucosal damage.
During treatment, no new oral lesions appeared and their development was limited. After 2 weeks from the start of the recommended general and topical treatment, the lesions on the oral mucosa healed and the swelling of the tongue significantly decreased, but visible areas of smoothing of filiform papillae on the tongue with the character of a geographic tongue remained. Patient has been under observation for 1.5 years. Small lesions on the tongue in the nature of a geographic tongue still persist, causing periodic slight hypersensitivity to foods and temperature changes.
In topical treatment painful lesions on the oral mucosa are most commonly treated with antibacterial, analgesic, anti-inflammatory, anti-fungal agents, as well as antiseptic rinses and herbal infusions [2].
Formulations used for topical treatment of lesions should act quickly, reducing pain and providing protection against infection. When ordering topical treatment, we have the opportunity to match the form of the preparation to the type of lesion in the oral cavity. For isolated lesions, coating preparations in gel form that isolate the damaged mucosal surface from external factors will work well [2,11,12].
However, in case of diffuse lesions, covering a large area of the oral mucosa, tongue and often located in inaccessible areas, oral rinses with analgesic and anti-inflammatory properties will be a better option [2,14].
For oral inflammation, in addition to systemic treatment, it is very important to implement local treatment as soon as possible. It aims to reduce pain, inflammation, reduce the possibility of opportunistic infections, promote healing of the damaged mucosa and enable the patient to perform activities of daily living.
Dr. n. med. Malgorzata Bartoszcze-Tomaszewska – LARDENT Dental Center in Lublin